Migraine comorbidity
By: Ria Bhola, Headache Nurse Specialist
What is a comorbidity?
A comorbidity refers to the presence of two or more chronic medical conditions occurring together at a higher than coincidental rate, compared to the general population. Migraine is a complex brain disorder, and it is common to have at least one comorbidity. However, having migraine does not mean you have or will develop a comorbid condition.
Several conditions are considered to be comorbid with migraine, but we don’t yet fully understand the underlying process linking them.
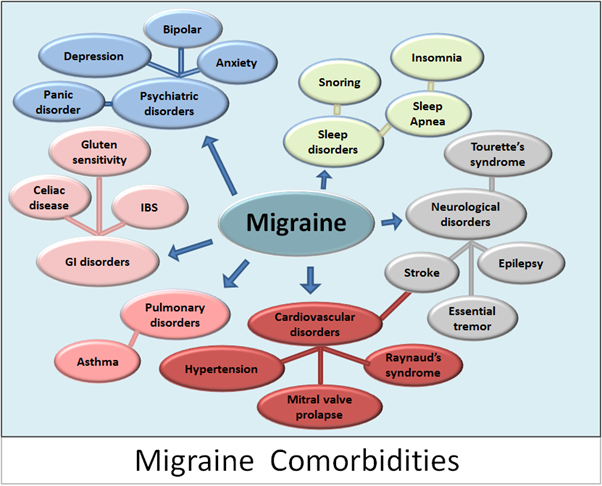
Credit: 7Mike7000, Wikimedia Commons, CC BY-SA 3.0
How do comorbidities develop?
Conditions are believed to be comorbid through a variety of mechanisms. They may be comorbid because of shared genetic or other factors, that will increase the risk of developing both conditions. There may be an underlying cause that triggers both conditions. However, it is not clear why some conditions are comorbid with migraine, and it is important to remember that having migraine does not mean you will develop a comorbid condition. We can consider two examples, epilepsy and fibromyalgia.
A comorbid link between migraine and epilepsy?
Epilepsy is a condition related to abnormal brain activity that results in different types of seizures. Both migraine and epilepsy occur when brain cells become overexcited. However, migraine is more common. Migraine attacks last hours or days and migraine is more common in females, whereas epileptic seizures typically lasts seconds to minutes, affect men and women equally and are less common. Some people have a headache after a seizure and although very rare, migraine with aura has been reported to trigger a seizure (referred to as migralepsy).
A comorbid link between migraine and fibromyalgia?
Fibromyalgia is a chronic condition that features musculoskeletal pain (pain in the muscles, bones and joints). It can cause fatigue and affect sleep and mood. Some symptoms are common to fibromyalgia and migraine such as headache, sensitivity to light and noise and stomach discomfort. Both are more common in women. However, a direct link between the two conditions is not known.
Why does it matter?
The significance of comorbid conditions is probably more important when selecting treatments. Although the links and causes are not well understood, discussing the symptoms and having a diagnosis is important. Treating each condition is nearly always recommended since one can either make the other worse, or to improve overall function, both will require treatment.
- You should always ask your doctor or specialist about the possible side effects of medications offered. You may then consider whether to avoid certain medicines that may worsen symptoms or be particularly careful and slower when increasing doses to reduce the chances of developing side effects.
- For example, a tricyclic antidepressant such as amitriptyline can help migraine, sleep and mood but may cause tiredness and worsen fatigue the following day. This does not necessarily mean it should be avoided. Taking the medicine earlier in the evening, or perhaps trying a different medication in that class (e.g. nortriptyline), may be more suitable and better tolerated.
- A non-drug treatment such as a dietary supplement, acupuncture and lifestyle changes may be preferred in the first instance. This may depend on the severity and impact of symptoms.
- In some cases, a single treatment could treat both conditions. This could limit the number of medicines needed and so reduce possible side effects, medicine interactions and brain fog.
- For others, the preferred preventive treatment may be an injectable option used monthly or quarterly to avoid daily exposure to a tablet, if side effects become an issue (e.g., CGRP mAbs, Botox, GON).
Managing migraine and a comorbidity
As migraine is very common, many people with a range of other medical conditions will find there is often an overlap, which does not mean that one condition has caused the other.
If you have migraine and comorbidities, it is recommended you see a headache specialist or neurologist for review and treatment. They may better understand the conditions, have access to more treatments and be able to offer a treatment plan that is effective and takes all conditions and symptoms into consideration.
Learn more about migraine treatments here. Find out more about getting a referral to a neurologist or headache specialist here.


